Platelet-rich fibrin (PRF) facials are regenerative treatments that use components derived from a patient’s own blood to support skin rejuvenation. The technique is sometimes used in aesthetic dentistry and facial aesthetics to improve skin quality, stimulate collagen production, and support natural tissue regeneration.
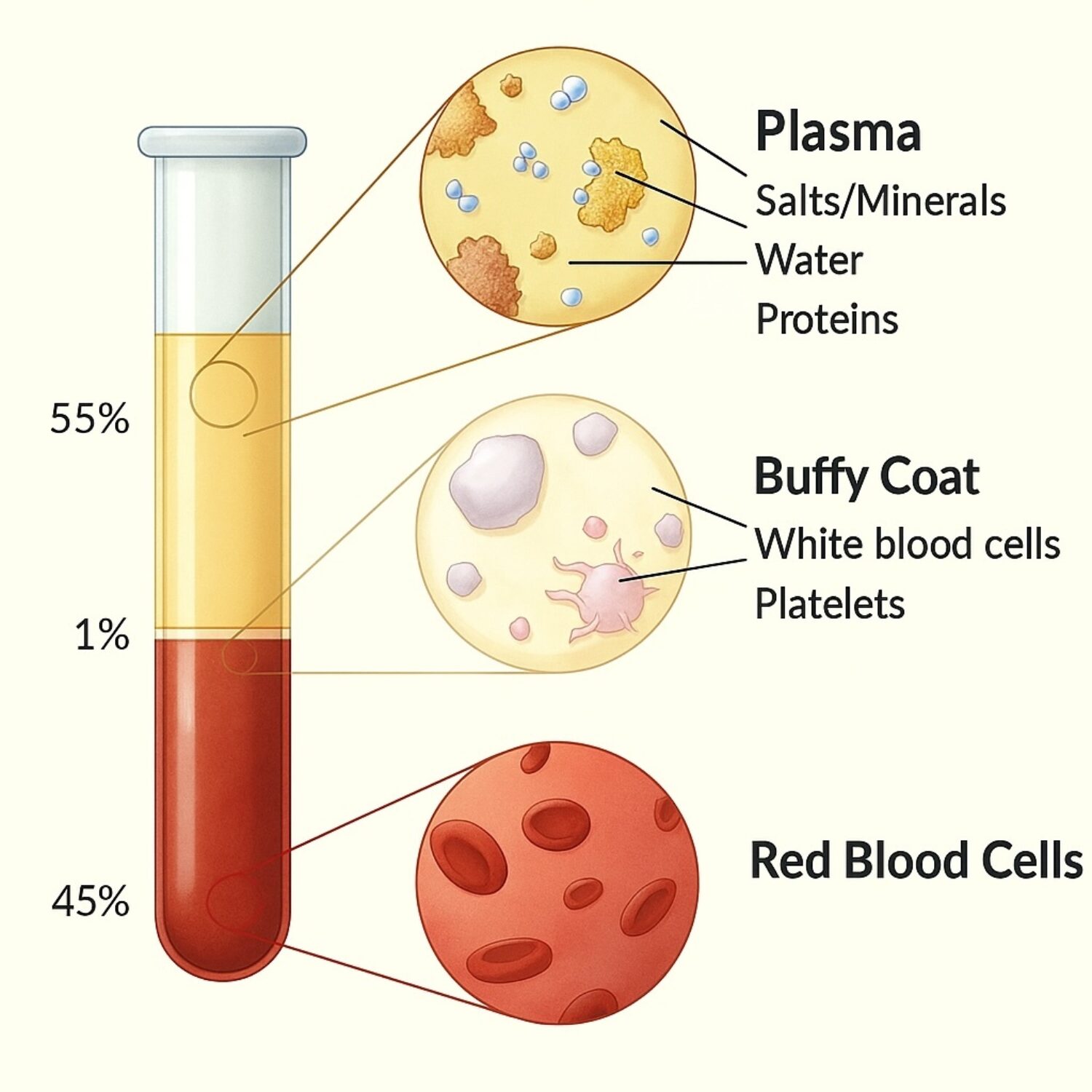
PRF is derived from a small blood sample that is processed to concentrate platelets and growth factors. These biological components can then be applied or injected into the skin to encourage healing and regeneration.
This article explains what PRF facials are, how they work, what the treatment involves, and who may be suitable for this type of facial rejuvenation procedure.
PRF is a blood-derived concentrate created using a patient’s own blood sample. It contains platelets, fibrin, and growth factors that contribute to collagen synthesis, tissue repair, and skin remodelling.
PRF belongs to the same family of regenerative treatments as Platelet-Rich Plasma (PRP). However, PRF is prepared using lower centrifugation speeds and does not contain anticoagulants. As a result, it forms a fibrin matrix that gradually releases growth factors over time, which may support more sustained regenerative effects compared with PRP.
Originally used in dentistry and orthopaedics to aid healing, PRF is now increasingly utilised for facial rejuvenation in clinical aesthetic settings.
Unlike PRP, PRF does not use anticoagulants, allowing the fibrin matrix to form naturally. This matrix gradually releases growth factors, supporting skin healing and collagen stimulation over time.
Application methods include:
- Microneedling with PRF – applying PRF to microchannels created in the skin
- Targeted injections – introducing PRF into specific areas, such as under the eyes or around folds
Although PRF is derived from the patient’s own blood, it remains a medical procedure requiring strict handling protocols. Performing PRF treatments in a clinical environment helps to:
- Maintain sterility during blood collection and preparation
- Reduce the risk of contamination
- Ensure accurate application using sterile equipment
- Tailor treatment based on individual anatomy and clinical assessment
These factors are essential for both safety and predictable outcomes.
A typical PRF facial session follows several structured steps:
- Consultation – A clinical review of medical history, skin concerns, and treatment goals to ensure suitability and develop a tailored plan.
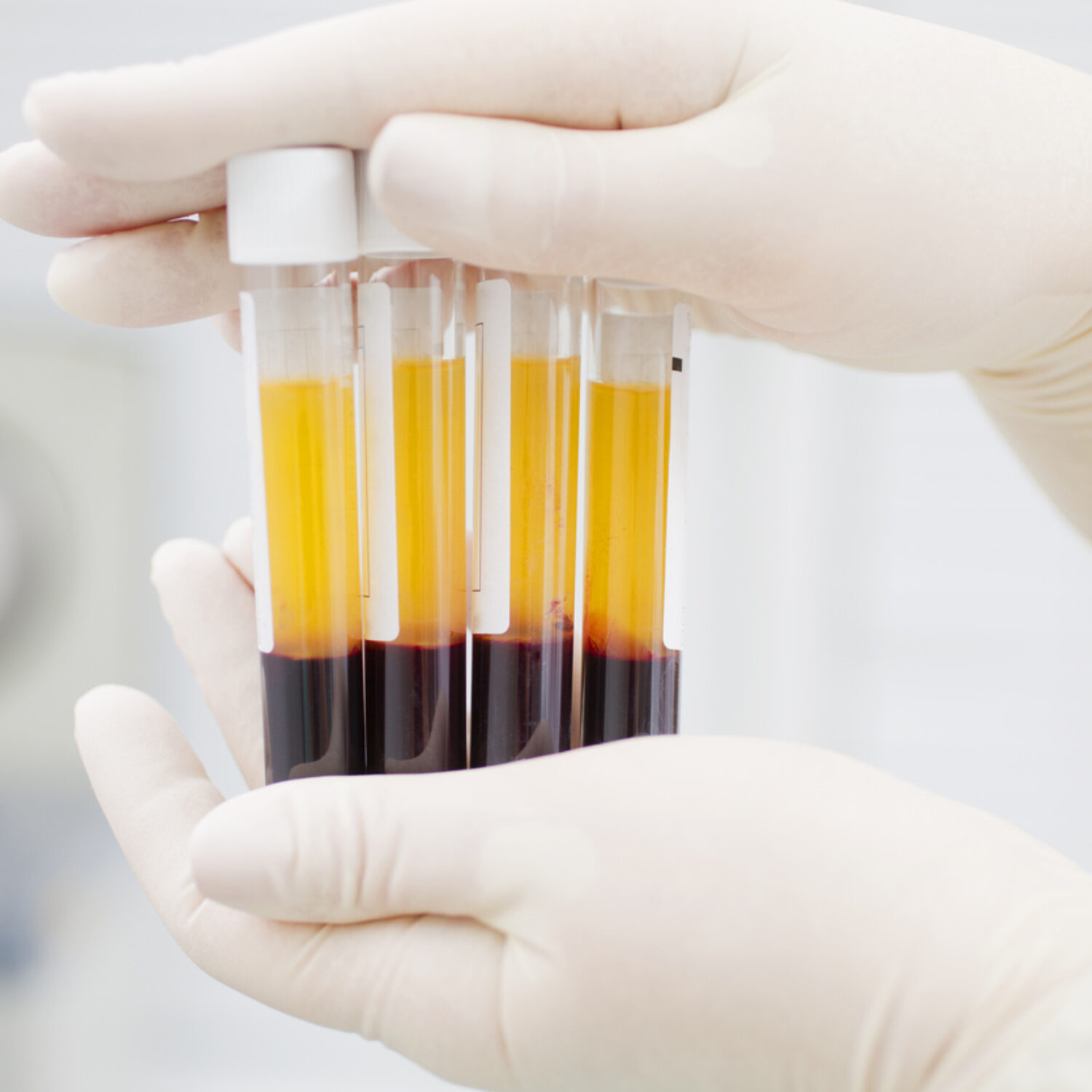
- Blood Draw – A small sample is collected, similar to a routine blood test.
- Centrifuge Preparation – The sample is processed without additives to separate PRF from other blood components.
- Application – PRF is introduced into the skin through microneedling or targeted injections, depending on the areas being treated.
- Recovery – Mild redness or swelling may occur, typically resolving within 24 hours.
Treatment duration usually ranges from 45 to 90 minutes, depending on the number and size of areas treated.
PRF treatments are usually planned as a structured course to achieve and maintain results:
- Initial course: 2–3 sessions, spaced 4–6 weeks apart.
- Maintenance: Every 6–12 months, tailored to the individual’s skin condition and response.
These intervals may vary based on clinical assessment and personal treatment goals.
Appropriate aftercare supports healing and helps sustain the regenerative benefits of PRF. Common recommendations include:
- Daily application of a high-SPF sunscreen to protect regenerating skin.
- Use of hydrating products such as hyaluronic acid to maintain moisture balance.
- Incorporation of antioxidant or peptide serums to support collagen synthesis.
- Following a gentle skincare routine, avoiding exfoliants and irritants for several days post-treatment.
- Follow-up sessions as advised to promote ongoing collagen production and maintain results.
PRF represents a natural, evidence-based approach to supporting skin health and rejuvenation. By using the body’s own platelets and growth factors in a controlled clinical environment, it offers a regenerative alternative to synthetic injectables.
As with any medical procedure, consultation with qualified practitioners is essential to assess suitability, discuss realistic expectations, and develop a personalised treatment plan.