Tooth decay in adults is caused by acids produced by plaque bacteria that gradually damage the tooth. Early decay may sometimes be stabilised or reversed with fluoride and improved oral care, but once a cavity forms, it usually requires treatment such as a filling. Early diagnosis matters because treatment is typically simpler and less invasive when caught early.

What is tooth decay?
Tooth decay, also called dental caries or a cavity, is the breakdown of tooth structure caused by acid produced by bacteria in plaque. These bacteria feed on sugars in food and drink, creating acids that gradually weaken the tooth.
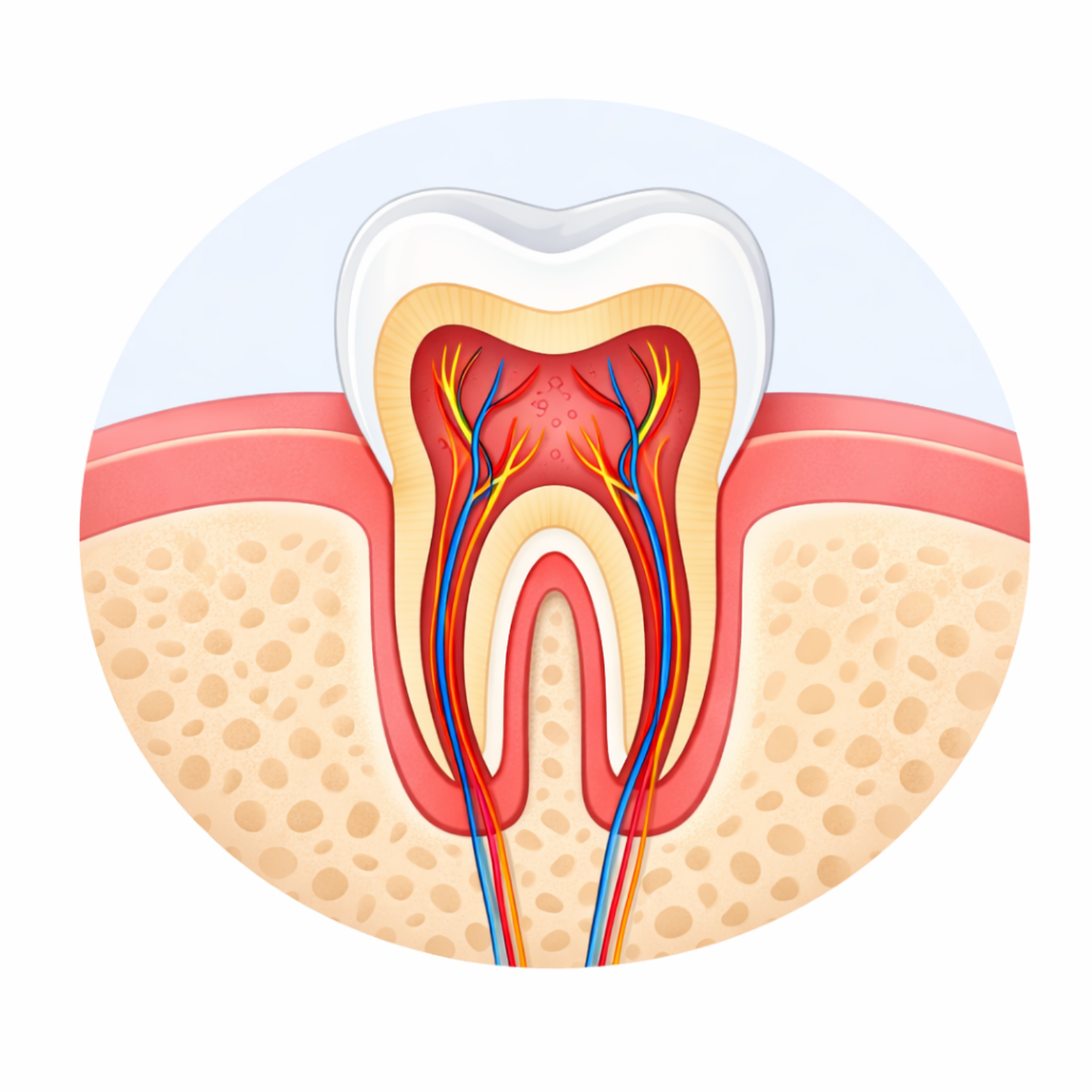
A tooth has three main layers:
- Enamel – the hard outer surface
- Dentine – the softer layer beneath
- Pulp – the inner part containing the nerve and blood supply
Decay usually starts in the enamel and progresses deeper if not treated.
Can tooth decay be reversed?
Early tooth decay can sometimes be stabilised or remineralised using fluoride, improved oral hygiene, and reducing sugar intake. However, once a physical cavity (hole) has formed, the tooth cannot repair itself and will usually require treatment.
- Early enamel damage → may be managed without drilling
- Visible cavity → usually needs a filling
- Pain or swelling → may indicate advanced decay
A useful rule of thumb is that if there is already a physical hole in the tooth, it cannot heal on its own and will require treatment.
What are the signs of tooth decay in adults?
Early tooth decay often has no symptoms. It is common for patients to have decay without pain, even when it is relatively advanced. As it progresses, signs may include:
- Sensitivity to cold, sweet, or hot foods and drinks
- White, brown, or black marks on teeth
- Visible holes or rough areas
- Food trapping between teeth
- Pain when biting
- Ongoing toothache
- Bad taste or swelling in more advanced cases
When to act:
- Pain → urgent assessment
- Swelling → urgent care
- Food trapping or sensitivity → book a check-up
What causes tooth decay?
Tooth decay develops when bacteria in plaque feed on sugars and produce acid. Repeated acid attacks weaken the tooth surface over time. Some foods are more likely to cause decay than others. For example, sticky sweets tend to stay on the teeth for longer, increasing the time bacteria can produce acid. Over time, if these acid attacks happen frequently, the tooth does not have enough time to recover, and decay develops.
Common risk factors include:
- Frequent sugary snacks or drinks
- Inadequate brushing or cleaning between teeth
- Dry mouth
- Deep grooves or crowded teeth
- Gum recession exposing roots
- Dental appliances that trap plaque

Who is more at risk?
You may be at higher risk if you have:
- Frequent sugar intake
- Poor plaque control
- Dry mouth from medications or health conditions
- Receding gums
- Braces, bridges, or dentures
- Previous history of decay
How does tooth decay progress?
| Stage | What happens | Symptoms | Typical treatment |
|---|---|---|---|
| Early enamel | Mineral loss | None | Fluoride, monitoring |
| Enamel cavity | Small hole forms | Mild sensitivity | Filling |
| Dentine decay | Spreads deeper | Sensitivity, discomfort | Filling or onlay |
| Pulp involvement | Nerve affected | Pain, infection | Root canal or extraction |
Does tooth decay always hurt?
No. Early tooth decay is usually painless. Pain becomes more likely as decay reaches deeper layers of the tooth.
Symptoms may include:
- Sensitivity to hot, cold, or sweet
- Discomfort when eating
- Sharp pain when biting
- Persistent toothache in advanced stages
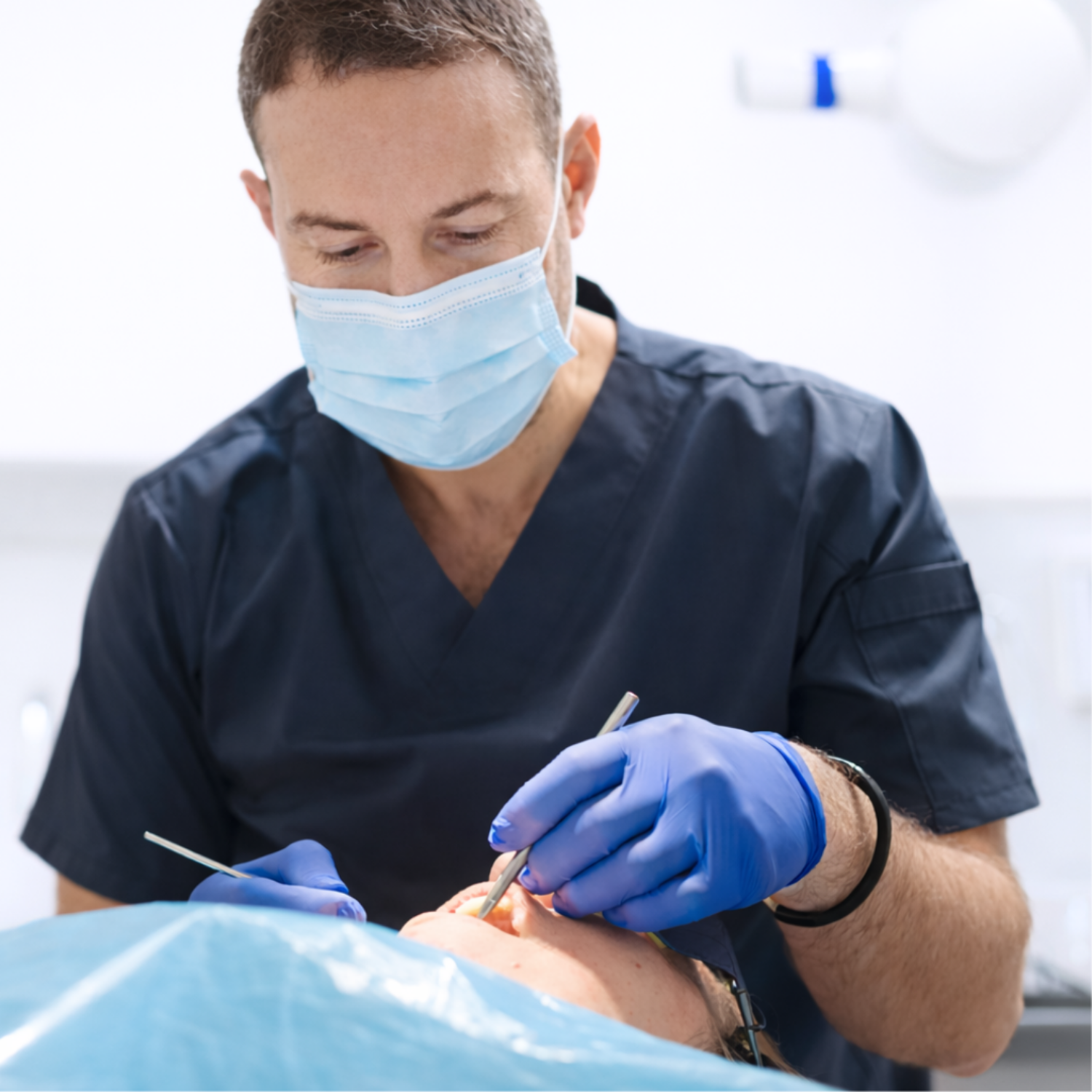
How do dentists treat tooth decay?
Treatment depends on how advanced the decay is and how much of the tooth can be preserved. In some cases, very early decay may be monitored rather than treated immediately, especially if it is not progressing and risk factors are well controlled.
- Early stage: Fluoride treatment, monitoring, and changes to oral hygiene and diet
- Fillings: Used to repair small to moderate cavities
- Inlays or onlays: Suitable for larger areas where a filling is not strong enough
- Crowns: Used when a tooth is significantly weakened or heavily restored
- Root canal treatment: Needed if the decay reaches the nerve and causes infection
- Extraction: Considered when the tooth cannot be predictably restored
When is tooth decay considered an emergency?
Seek prompt dental care if you experience:
- Persistent or severe toothache
- Swelling of the gum, face, or jaw
- Bad taste or discharge
- Pain when biting
- Broken tooth with pain
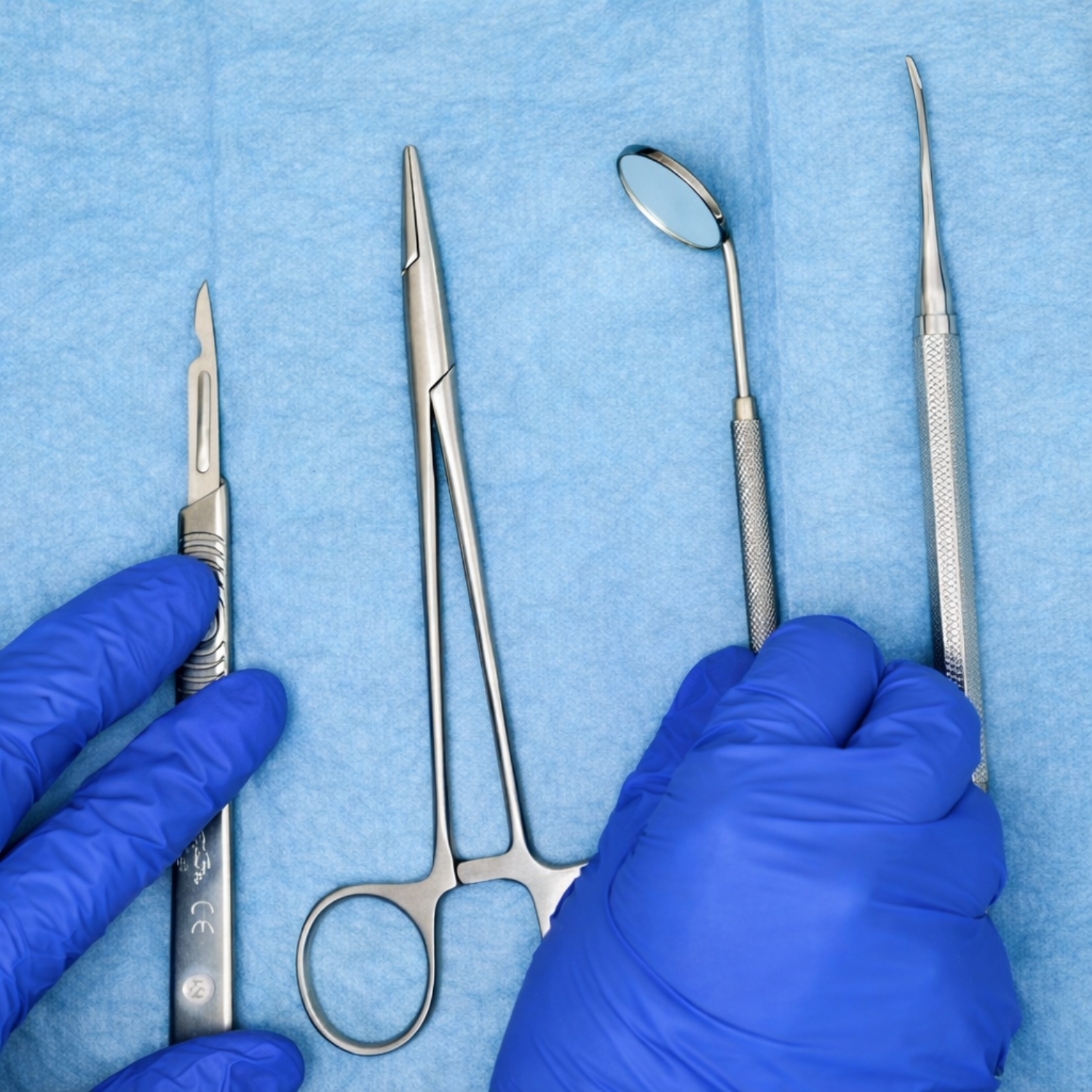
What happens if tooth decay is left untreated?
Untreated decay can lead to:
- Increasing pain
- Infection or abscess
- Tooth fracture
- Need for root canal treatment
- Tooth loss
If you notice early signs, having the tooth assessed sooner usually means simpler, less invasive treatment.
How can adults reduce the risk of tooth decay?
Focus on three key areas:
1. Clean effectively
Brush twice daily with fluoride toothpaste
Spit, don’t rinse after brushing
Use interdental brushes or floss daily
2. Reduce sugar frequency
Limit snacking
Keep sugary foods and drinks to mealtimes
It is the frequency of sugar exposure, rather than just the amount, that has the greatest impact on decay risk.
3. Use fluoride consistently
Use fluoride toothpaste daily
Consider higher-fluoride products if advised
Conclusion
Tooth decay in adults is common but often manageable when detected early. Early-stage damage may sometimes be stabilised, but established cavities usually require treatment. If you notice sensitivity, food trapping, or pain, having the tooth assessed sooner usually means simpler, less invasive treatment.
More
from the blog
Blog /Advice
Why Don’t My Teeth Line Up Properly?
Understanding Bite Problems, Misalignment and Treatment Options
Read moreBlog /Advice
Children’s Dental Space Maintainers
Protecting space for developing permanent teeth
Read more